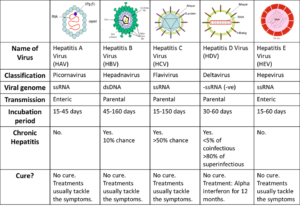
Hereditary clotting factor deficiencies. Single clotting factor deficiency. Factor I, II, V, VII, X, XI, XIII deficiency (autosomal) Factor VIII/IX deficiency (X-linked recessive) Factor XII deficiency (non-bleeding disorder) Multiple clotting factor deficiencies. F V + F VIII (autosomal recessive) Vitamin K dependent factors (F II, VII, IX, X) Von Willebrand Disease. Inherited platelet disorders. Wintrobe’s Clinical Hematology, 11th ed, 2004.
Bleeding disorders are a group of conditions that result when the blood cannot clot properly. In normal clotting, platelets, a type of blood cell, stick together and form a plug at the site of an injured blood vessel. Proteins in the blood called clotting factors then interact to form a fibrin clot, essentially a gel plug, which holds the platelets in place and allows healing to occur at the site of the injury while preventing blood from escaping the blood vessel. While too much clotting can lead to conditions such as heart attacks and strokes, the inability to form clots can be very dangerous as well, as it can result in excessive bleeding. Bleeding can result from either too few or abnormal platelets, abnormal or low amounts of clotting proteins, or abnormal blood vessels.
Hemophilia is perhaps the most well-known inherited bleeding disorder, although it is relatively rare. It affects mostly males.
Many more people are affected by von Willebrand disease, the most common inherited bleeding disorder in America caused by clotting proteins. Von Willebrand disease can affect both males and females. Platelet disorders are the most common cause of bleeding disorder and are usually acquired rather than inherited. You can find information on other bleeding disorders by following the links at the bottom of this page.
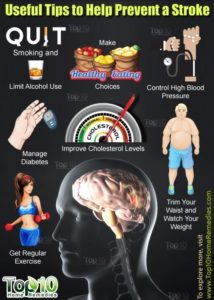
How do you know if your at risk?
Bleeding disorders such as hemophilia and von Willebrand disease result when the blood lacks certain clotting factors. These diseases are almost always inherited, although in rare cases they can develop later in life if the body forms antibodies that fight against the blood’s natural clotting factors. Individuals and pregnant women with a family history of bleeding disorders should talk to their doctors about detection and treatment. Symptoms of bleeding disorders may include:
- Easy bruising
- Bleeding gums
- Heavy bleeding from small cuts or dental work
- Unexplained nosebleeds
- Heavy menstrual bleeding
- Bleeding into joints
- Excessive bleeding following surgery
What is Hemophilia and how is it treated?
Hemophilia is a rare, inherited bleeding disorder that can range from mild to severe, depending on how much clotting factor is present in the blood. Hemophilia is classified as type A or type B, based on which type of clotting factor is lacking (factor VIII in type A and factor IX in type B). Hemophilia results from a genetic defect found on the X chromosome. Women have two X chromosomes. Women who have one X chromosome with the defective gene are termed carriers and they can pass the disease onto their sons. Due to random chromosome activation, some women carriers may range from asymptomatic to symptomatic depending on how much of their factor VIII or IX is inactivated. In fact, some women may have “mild hemophilia,” though this is less common. Men have one X and one Y chromosome, so if their X chromosome has the defective gene, they will have hemophilia.
Because blood does not clot properly without enough clotting factor, any cut or injury carries the risk of excessive bleeding. In addition, people with hemophilia may suffer from internal bleeding that can damage joints, organs, and tissues over time.
In the past, people with hemophilia were treated with transfusions of factor VIII obtained from donor blood, but by the early 1980s these products were discovered to be transmitting blood-borne viruses, including hepatitis and HIV. Thanks to improved screening techniques, and a major breakthrough that enabled scientists to create synthetic blood factors in the laboratory by cloning the genes responsible for specific clotting factors, today’s factor-replacement therapies are pure and much safer than ever before.
What Is von Willebrand Disease and How Is It Treated?
Von Willebrand disease is an inherited condition that results when the blood lacks functioning von Willebrand factor, a protein that helps the blood to clot and also carries another clotting protein, factor VIII. It is usually milder than hemophilia and can affect both males and females. Women are especially affected by von WIllebrand disease during menses. Von Willebrand disease is classified into three different types (Types 1, 2, and 3), based on the levels of von Willebrand factor and factor VIII activity in the blood. Type 1 is the mildest and most common form; Type 3 is the most severe and least common form.
With early diagnosis, people with von Willebrand disease can lead normal, active lives. People with mild cases may not require treatment, but should avoid taking drugs that could aggravate bleeding, such as aspirin and ibuprofen, without first consulting with a doctor. More serious cases may be treated with drugs that increase the level of von Willebrand factor in the blood or with infusions of blood factor concentrates. It is important for people with von Willebrand disease to consult with their doctors before having surgery, having dental work, or giving birth, so that proper precautions can be taken to prevent excessive bleeding. You may be referred to a hematologist, a doctor who specializes in the treatment of blood disorders.