1. BOATING ACCIDENTS
People’s biggest mistake by far is drinking and boating. People get out there and drink alcohol all day in the sun, and you end up with the same accidents you have with driving — with the added risks of falling out of boats, getting hit by propellers, and drowning.
It’s also easy to get lax about life jackets. Kids need to have them on all the time. Even if having them under the seat fulfills the law, in an accident, chances are anyone who doesn’t know how to swim won’t be able to get to them in time. When you are going to be out on a boat or at the beach with a child, you take on the responsibility to maintain the safety of that child and basic lifesaving skills are a must, not a luxury; especially for parents. The courses are easy, usually just one day or half a day and you may save your child’s LIFE or the child you take the responsibility in caring for. There’s no mouth-to-mouth [resuscitation] anymore if you are not trained — just chest compressions but if you get BCLS certified (basic care in life support) your CPR certified.
You can find first aid, cardiopulmonary resuscitation (CPR), and other emergency lifesaving courses near you with the American Heart Association’s ECC (Emergency Cardiovascular Care) Class Connector tool online at americanheart.org. or near you where you live.
2. Mower Injuries
We know almost every homeowner loves the sight of a pristine, neatly mowed yard. But in their haste to get that lawn in shape, some people forget to take precautions. “In the warmer months we see lots of mower injuries to toes, hands, and fingers getting caught in blades, and things like rocks and sticks getting flung out of them. People will start tinkering with the mower and reach under it to unclog it, and forget there’s a spinning blade there or take the key out when going under to see what clogged the blade from working. Those can be preventative moves and result in hideous injuries for some permanent and with others temporary.
They’re also hard to repair, because not only can whirling blades cause complex lacerations and fractures, but they can bury contaminants like grass and dirt in the wound putting the wound at risk for infection. To be safe:
Wear closed-toed shoes — preferably with a steel toe — when you mow, along with goggles or sunglasses, gloves, and long pants that will protect you from flying debris.
Keep kids away from the push mower and off the riding mower. Riding mowers are not just another ride-on toy.
Get a professional to service your mower or learn how to do it properly. Important: Disconnect the spark plug to prevent it from accidentally starting. Turning a push mower’s blade manually can ignite the engine.
3. Dehydration Disasters
You’ve romped outdoors with the kids all day, and your water bottle ran dry long ago. Suddenly you feel dizzy and lightheaded, and your mouth tastes like cotton. You’re dehydrated — meaning you haven’t taken in enough fluids to replace those you’ve been sweating out.
People can get dehydrated any time of year, but it’s much more common in the summer months, when they are active outdoors in the warm sun. Heatstroke is the most severe form of dehydration. That’s when your internal temperature rises to dangerously high levels. Your skin gets hot, but you stop sweating. Someone with heatstroke may pass out, have hallucinations, or suffer seizures.
Preventing dehydration and heatstroke is so easy: Drink plenty of fluids, especially water, take regular breaks in the shade, and try to schedule your most vigorous outdoor activities for times when the heat isn’t so strong, such as early morning or late afternoon.
For persons suffering more serious dehydration or heatstroke, get them indoors, have them lie down, and cool them off with ice packs and cool cloths. Someone who is seriously affected by the heat may need intravenous fluids in the ER.
4. Sunburn
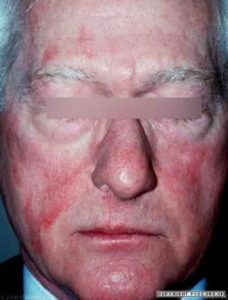
With all the skin cancer warnings, you’d think Americans would be getting fewer sunburns, not more. But you’d be wrong. The percentage of adults nationwide who got at least one sunburn during the preceding year rose from 31.8% in 1999 to 33.7% in 2004, according to the CDC.
Your risk for melanoma doubles if you’ve had just five sunburns in your life. A sunburn is a first-degree burn, right up there with thermal burns. Also, we even see some second-degree thermal burns, often when people are out drinking or falling asleep in the sun and don’t realize how long they’ve been out there.
In addition to practicing “safe sun” — wearing sunscreen that protects against both UVB and UVA rays, long-sleeved shirts, and wide-brimmed hats, and staying out of blistering midday rays — there are things you can do to treat a severe sunburn, Stanton says:
-Drink water or juice to replace fluids you lost while sweating in the hot sun.
-Soak the burn in cool water for a few minutes or put a cool, wet cloth on it.
-Take an over-the-counter pain reliever, such as acetaminophen.
-Treatitching with an OTC antihistamine cream or a spray like diphenhydramine (such as Benadryl), which helps block the inflammatory reaction.
-Apply an antibiotic ointment or an aloe cream with emollients that soften and soothe the skin directly to the burned area.
-You’re going to have a pretty miserable 12 to 24 hours with the initial symptoms no matter what you do.
5. Picnic Poisoning
Food poisoning puts about 300,000 people in the hospital every year, hitting its peak in the summer months. You don’t want diarrhea to be the souvenir of your family’s annual summer picnic.
Anything that has mayonnaise, dairy, or eggs in it and any meat products can develop some pretty nasty bacteria after only a couple of hours unrefrigerated. Every summer we’ll have five or six people coming in from the same reunion or family picnic with food poisoning symptoms.
To prevent food poisoning, follow the U.S. Department of Agriculture’s advice to:
- Clean — Wash your hands as well as the surfaces where you’ll be preparing foods.
- Separate — Wrap raw meat securely and keep it stored away from other food items.
- Cook — Bring along a meat thermometer. Grilling meat browns it very fast on the outside, but that doesn’t mean it’s safe on the inside. Steaks should be cooked to a minimum internal temperature of 145 degrees, ground beef and pork to 160 degrees, and poultry to 165 degrees.
- Chill — Keep everything refrigerated as long as possible. Store perishable picnic items in an insulated cooler packed with ice, and follow the “last in, first out” rule — whatever you’re going to eat first should go at the top of the cooler.
Mild cases of food poisoning can be cared for at home, Stanton says. Avoid solid foods, and stick with small, frequent drinks of clear liquid to stay hydrated. Once the nausea and vomiting have eased, you can try bringing food back into your diet — slowly and in small, bland portions (Grandma knew what she was talking about when she recommended tea and toast to settle an upset stomach). If symptoms persist for more than a couple days (or more than 24 hours in small kids), see a doctor.
6. Fireworks
Independence Day arrives. Many people love fireworks, but fireworks don’t necessarily love them back. Nearly 9,000 individuals were injured by fireworks in 2009, according to the U.S. Fire Administration, and two were killed. We see pretty significant hand and eye injuries from fireworks every summer. The safest way to watch fireworks is at a professionally sponsored display. At least six states ban all consumer fireworks, and several more allow them only with limitations. But if you can buy fireworks legally and want to set off a few at home, take these precautions:
- Keep a hose or fire extinguisher handy to put out small fires.
- Keep children away from fireworks.
- Everybody loves to give sparklers to kids, but they burn very hot and can cause significant eye injuries. In fact, a sparkler can burn as hot as 2,000 degrees — hot enough to melt some types of metals. They can go off quickly and cause burns or just explode in your hand.
To care for a fireworks burn, wrap it in a clean towel or T-shirt saturated with cool water and get to an emergency room to have the injury checked out.