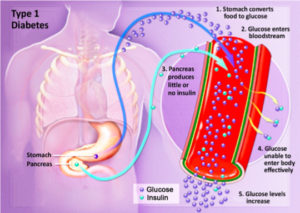
Diabetes Mellitus (DM) is a complex chronic disease involving disorders in carbohydrate, protein, and fat metabolism and the development of macro-vascular, micro-vascular, neurological complications that don’t occur over a few nights or weeks or months. It is a metabolic disorder in where the pancreas organ ends up causing many disruptions in proper working of our body. The pancreas is both an endocrine and exocrine gland.
The problem with diabetes is due to the endocrine part of the pancreas not working properly. More than 1 million islet cells are located throughout this organ. The three types of endocrine cells that the pancreas excretes into our blood stream are alpha, beta, and delta cells. The alpha cells secrete glucagon (stored glucose), beta secrete insulin, and delta secrete gastrin and pancreatic somatostatin.
A person with DM has minimal or no beta cells secreted from the pancreas, which shows minimal or no insulin excreted in the person’s bloodstream. Insulin is necessary for the transport of glucose, amino acids, potassium, and phosphate across the cell membrane getting these chemical elements into the cell. When getting these elements into the cells it is like the cell eating a meal and the glucose, being one of the ingredients in the meal, is used for energy=fuel to our body; the glucose inside the cells gets carried to all our tissues in the body to allow the glucose to be utilized into all our tissues so they can do their functions (Ex. Getting glucose into the muscle tissue allows the muscles to have the energy to do the range of motion in letting us do our daily activities of living, like as simple as type or walk). The problem with diabetes is the glucose doesn’t have the insulin being sent into the bloodstream by the pancreas to transfer the glucose across the cell membrane to be distributed as just discussed. Instead what results is a high glucose levels in the blood stream outside the cells causing hyperglycemia. Remember when a doctor has you go to the lab or even in his office getting blood drawn from your arm to check blood levels of electrolytes (like glucose, potassium, sodium) or even drug levels, its measuring only these elements outside the cell. We cannot measure the levels of these elements inside the cell or we would have to break the cell destroying it which makes no logic or help in diagnosing.
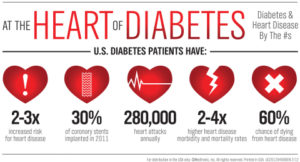
It should be apparent that when there is a deficit of insulin, as in DM, hyperglycemia with increased fat metabolism and decreased protein synthesis occur ( Our body being exposed to this type of environment over years causes the development of many chronic conditions that would not have occurred if DM never took place in the body, all due to high glucose levels starting with not being properly displaced in the body as it should be normally since insulin loss didn’t allow the glucose to go into the cells but remained outside the cells.).
People with normal metabolism upon awaking and before breakfast are able to maintain blood glucose levels in the AM ranging from 60 to 110mg/dl. After eating food the non-diabetic’s blood glucose may rise to 120-140 mg/dl after eating (postprandial), but these then rapidly return back to normal. The reason for this happening is you eat food, it reaches the stomach, digestion takes place during digestion the stomach breakes down fats, carbohydrates, and sugars from compound sugars to simple sugars (fructose and glucose). Than the sugars transfer from the stomach into the bloodstream causing an increase in sugar levels. Now, your body uses the sugar it needs at that time throughout the entire body for energy and if still extra sugar left in the bloodstream that isn’t needed at that time to be utilized it now needs to go somewhere out of the bloodstream to allow the glucose blood level to get back between 60-110mg/dl. That extra glucose first gets stored up in the liver 60-80%. How this happens is the extra glucose in the blood stream not needed now fills up the liver (like filling up your gas tank) but limits the amount it can take. When the glucose goes in the liver it goes from active sugar to inactive by getting converted from glucose to glycogen=inactive sugar now. Now when the liver can store no more then the extra glucose left in the bloodstream after all tissues utilized the digested sugar sent to the bloodstream after digestion and the next place for storage gets stored in our fat tissue=fat storage=weight increase. That is the logic behind eating small meals properly dispensed with protein/CHOs/sugars/fat every 6hrs. This limits the amount of food to digest down to prevent excess sugar in the bloodstream preventing hyperglycemia from occurring and most of your small meal if not all is utilized by our muscle tissues preventing both hyperglycemia and high fat distribution of the glucose to prevent weight increase, also.
Unfortunately this doesn’t take place with a diabetic since there is very little or no insulin being released by the pancreas and over time due to the high blood glucose blood levels (called hyperglycemia) problems arise in the body over years. When diabetes occurs there is a resolution and you have the disease the rest of your life. You need to control your glucose level through proper dieting for a diabetic with balancing exercise and rest. Exercise uses up your glucose also in the body. Increase activity the body needs energy the gas for the body is glucose, like gas in our auto vehicles in the tank.
TWO TYPES OF Diabetes Mellitus:
1.)Diabetes I
2.) Diabetes ll
We have risk factors that can cause disease/illness; there are unmodified and modified risk factors.
With unmodified risk factors we have no control in them, which are 4 and these are:
1-Heredity 2-Sex 3-Age 4-Race.
Now modified risk factors which are factors we can control. They are
1.)Weight 2.)Diet 3.)Health Habits (which play a big role in why many people get diabetes II) 5.)Physical Inactivity 6.)Hyperlipidemia and Hypertension
Stayed tune for part III tomorrow on more knowledge of this disease.