Diagnostic Tests for Amyloidosis:
*1. First your doctor would do a thorough medical exam with blood/urine tests searching for clues of high protein where it shouldn’t belong or certain liver or thyroid abnormal findings. The MD will follow with further diagnostic tooling especially if these findings show up in blood/urine tests. Common blood exams used are BNP (basic natriuretic peptide). BNP is a substance secreted from the ventricles or lower chambers of the heart in response to stress and changes in pressure that occur when to heart failure develops and worsens. The level of BNP in the blood increases when heart failure symptoms worsen, and decreases when heart failure condition is stable. It is not so much elevated over the norm but more with this disease patients the MD will see where the BNP level was at last visit & compare.
Another blood test is troponin and this gets released into the bloodstream when your heart is affected by amyloids.
*2. Second your MD may want to further diagnose for this disease through getting a tissue biopsy where the MD’s intent is to check for signs indicating this is highly possible for amyloidosis. The biopsy could be taken from your abdominal fat, bone marrow, or an organ such as your liver or kidney. Tissue analysis can help determine the type of amyloid deposit.
*3. Imaging Tests. Images taken of the organs that are affected by amloidosis can help the MD establish the intensity or stage your disease is at. There are 2 most commonly imaging tests used and can diagnose the disease early. There is the echocardiogram test, sound wave imaging of the heart, that will be used to assess the size and functioning capability level of the heart. Another test is a MRI of the heart (magnetic residence imaging). Other imaging tests can evaluate the extent of amyloidosis in the liver or spleen.
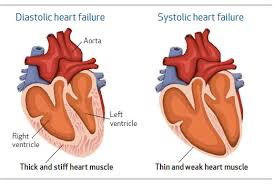
When the heart chambers become filled with amyloids it thickens the walls of those chambers especially the lower chambers which can be picked up by the echocardiogram through the different angles of sound waves that go via the heart during this exam. Another thing that can be measured through the echocardiogram is your diagnostic function; that represents a measure of how stiff your heart is and how well is your heart actually functioning.
Another technique that can be used is strain imaging. This is also done through echocardiogram. This tells the doctor in more detail how much the muscle fibers in the heart are actually shortening and contracting. It measures certain parts of the heart in actually contracting and function. This is actually better in help diagnosing compared to just looking at ejection fraction, which is the amount of blood pumped out of the left ventricle chamber upon contraction of the heart (When he hear lub dub of the heart with a stethoscope that is the heart actually contracting. First the upper chamber on lub is contracting and on dub is the lower chambers contracting). This test is a specializing test and is not widely used but it is available in certain hospitals.
Ending line amyloidosis is a group of diseases in which one or more organ systems in the body accumulate abnormal proteins known as amyloid. The name amyloidosis was first used more than 150 years ago, but cases were described over 300 years ago. However, only in the past ¼ of a century have MD’s understood the specific make up and structure of amyloid proteins. Although amyloidosis is not a cancer but it is a serious condition. It is disabilitating and gets to life threatening. However, growing aware- ness of the condition seems to be leading to substantial new research and Rx alternatives.
There’s no cure unfortunately for amyloidosis. But treatments can help you manage your symptoms and limit the production of amyloid protein.
Treatment is usually aimed at eliminating the source of the abnormal precursor protein.
Primary amyloidosis (AL, amyloid light chain) is associated with a clonal plasma cell disease and the immunoglobulin light chains made by the abnormal plasma cells. AL also occurs in amyloidosis associated with multiple myeloma. Treatment involves chemotherapy or stem cell transplantation to eliminate the plasma cells (the source of the abnormal light chains).
Familial amyloidosis (AF) is associated with a genetic abnormality that can be inherited. AF causes the liver to make an abnormal form of a protein called transthyretin. The treatment for AF is liver transplantation.
Secondary amyloidosis (AA) is associated with inflammation and elevated levels of serum amyloid A caused by inflammation. Treatment involves elimination of the source of inflammation.
Through “The Amyloidosis Foundation” they provide over the world medical facilities/hospitals that major in this disease at http://www.amyloidosis.org/PatientPrograms/physiciansusa.html.
Hope this article has helped you in some way for yourself or family or friend in better understanding about the disease, knowing tests for it, and places majored with this unfortunate disease an expert can treat in a medical facility.