2 TYPES OF DM:
a.)Diabetes I & b.) Diabetes ll.
We have risk factors that can cause disease/illness; there are unmodified and modified risk factors.
With unmodified risk factors we have no control in them, which are 4 and these are:
1-Heredity 2-Sex 3-Age 4-Race.
Now modified risk factors are factors we can control, 3 of them that you can control: They are 1.)your weight 2.)diet 3.)health habits (which play a big role in why many people get diabetes II).
Look at what the Mayo Clinic (www.mayoclinic.com /health/diabetes)says about risk factors:
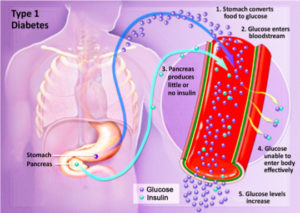
RISK FACTOR FOR TYPE DIABETES ONE:
Although the exact cause of type 1 diabetes is unknown, genetic factors can play a role. Your risk of developing type 1 diabetes increases if you have a parent or sibling who has type 1 diabetes. Based on research, we also know that genes account for less than half the risk of developing type1 disease. These findings suggest that there are other factors besides genes that influence the development of diabetes. We don’t know what these factors are, but a number of different theories exist. Environmental factors, such as exposure to a viral illness, also likely play some role in type 1 diabetes. Other factors that may increase your risk include:
The presence of damaging immune system cells that make autoantibodies. Sometimes family members of people with type 1 diabetes are tested for the presence of diabetes autoantibodies. If you have these autoantibodies, you have an increased risk of developing type 1 diabetes. But, not everyone who has these autoantibodies develops type 1.
Dietary factors. A number of dietary factors have been linked to an increased risk of type 1 diabetes, such as low vitamin D consumption; early exposure to cow’s milk or cow’s milk formula; or exposure to cereals before 4 months of age.
Race. Type 1 diabetes is more common in whites than in other races.
Geography. Certain countries, such as Finland and Sweden, have higher rates of type 1 diabetes.
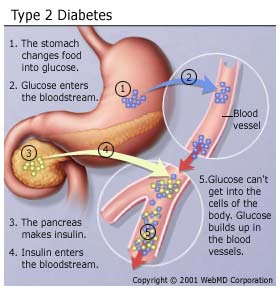
RISK FACTORS FOR DIABETES TYPE 2 AND PREDIABETES Researchers don’t fully understand why some people develop prediabetes and type 2 diabetes and others don’t. It’s clear that certain factors increase the risk, however, including:
Weight. The more fatty tissue you have, the more resistant your cells become to insulin.
Inactivity. The less active you are, the greater your risk. Physical activity helps you control your weight, uses up glucose as energy and makes your cells more sensitive to insulin. Exercising less than three times a week may increase your risk of type 2 diabetes.
Family history. Your risk increases if a parent or sibling has type 2 diabetes.
Race. Although it’s unclear why, people of certain races — including blacks, Hispanics, American Indians and Asians — are at higher risk.
Age. Your risk increases as you get older. This may be because you tend to exercise less, lose muscle mass and gain weight as you age. But type 2 diabetes is also increasing dramatically among children, adolescents and younger adults.
Gestational diabetes. If you developed gestational diabetes when you were pregnant, your risk of developing prediabetes and type 2 diabetes later increases. If you gave birth to a baby weighing more than 9 pounds (4 kilograms), you’re also at risk of type 2 diabetes.
Polycystic ovary syndrome. For women, having polycystic ovary syndrome — a common condition characterized by irregular menstrual periods, excess hair growth and obesity — increases the risk of diabetes.
High blood pressure. Having blood pressure over 140/90mm Hg is linked to an increased risk of type 2 diabetes.
Abnormal cholesterol levels. If you have low levels of high-density lipoprotein (HDL), or “good,” cholesterol, your risk of type 2 diabetes is higher. Low levels of HDL are defined as below 35 mg/dL.
High levels of triglycerides. Triglycerides are a fat carried in the blood. If your triglyceride levels are above 250 mg/dL, your risk of diabetes increases.
RISK FACTORS FOR GESTATIONAL DIABETES Any pregnant woman can develop gestational diabetes, but some women are at greater risk than are others. Risk factors for gestational diabetes include:
Age. Women older than age 25 are at increased risk.
Family or personal history. Your risk increases if you have prediabetes — a precursor to type 2 diabetes — or if a close family member, such as a parent or sibling, has type 2 diabetes. You’re also at greater risk if you had gestational diabetes during a previous pregnancy, if you delivered a very large baby or if you had an unexplained stillbirth.
Weight. Being overweight before pregnancy increases your risk.
Race. For reasons that aren’t clear, women who are black, Hispanic, American Indian or Asian are more likely to develop gestational diabetes.
The key not to get diabetes is taking Prevention Measures (especially regarding type II) but even diagnosed with diabetes there are measures you can take in helping to control the glucose and decreasing the chances of increasing the side effects of what it can cause to the human body organs overtime especially cardiac disease, kidney disease, neuropathy, retinopathy to blind from having hyperglycemia frequently over years; in time it thickens the blood making circulation difficulty effecting tissues furthest from the heart= feet/lower extremities where skin ulcers occur for not getting enough oxygen to the tissues in the feet or lower extremities that can lead to necrosis causing amputation of toes to foot to below knee amputation to even above knee amputation. It also increases chance of heart attack and stroke. PREVENTION first and CONTROL second when diagnosed with DM, is so vitally important.
So help control your diabetes through diet (eating a low glucose or sugar diet=1800 to 2000 calories a day as your m.d. prescribes for you), weight (get in therapeutic weight range), and practice healthy habits. In knowing how to prevent diabetes that would be to lose weight if obese by eating 6 low glycemic meals a day which allows low fat, low carbohydrates, low sugar keeping your baseline glucose at a steady level and low sugar level more on a regular basis with still treating yourself to occasional high glycemic meals when you’re in ideal weight.
This would definitely benefit you in prevention but if not or if diagnosed with diabetes always check with your doctor regarding diet, activity, and new health habits you may start, especially through any diet change and making alterations you need to do as your m.d. recommends.
Your doctor can guide you in what is the safest method for you especially if diagnosed with diseases.