Treatment for Multiple Sclerosis:
Today multiple sclerosis (MS) is not a curable disease. Effective strategies can help modify or slow the disease course, treat relapses (also called attacks or exacerbations), manage symptoms, improve function and safety, and address emotional health.
The model of comprehensive MS care involves the expertise of many different healthcare professionals — each contributing in a unique way to the management of the disease and the symptoms it can cause. Sometimes this team works within a single center, offering “one-stop shopping” for people with MS. More often, people are referred by their MS physician to other specialists in the community.
In either case, the goal is comprehensive=coordinated care to manage the disease and promote comfort, function, independence, health and wellness to its OPTIMAL LEVEL.
There are several types of MS:
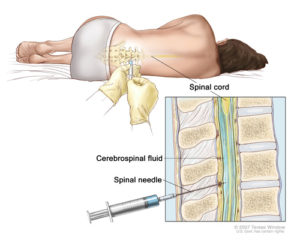
For an acute exacerbation of multiple sclerosis that can result in neurologic symptoms and increased disability or impairments in vision, strength or coordination, the preferred initial treatment is usually a type of steroid called a glucocorticoid. Patients who do not have a good response to steroidal therapy are often treated with plasma exchange. Plasma exchange is an extreme therapy that removes antibodies to myelin from the blood.
Some patients have disease that will have an acute exacerbation followed by a prolonged quiet period, which can last years or decades. This form of disease is referred to as relapsed remitting MS, or RRMS. Patients with relapsing MS=RRMS are often treated with immune-modulating drugs such as interferon or glatiramer acetate. Glatiramer is an exciting drug. It is a series of small proteins that are similar to myelin protein. It is thought to prompt the immune system to avoid attacking myelin.
Others have a disease that gets progressively worse over time.
There are two types of progressive disease:
1 In primary progressive MS, or PPMS, symptoms steadily worsen over time from the very beginning.
Progressive MS also referred to as disease-modifying therapies (DMTs).
Presently, these include 15 drug therapies to slow MS activity and progression, each of which is approved by the United States Food and Drug Administration (FDA) for relapsing forms of MS (and some are also approved for clinically isolated syndrome, prior to the diagnosis of MS). One of the medications, Ocrevus™ (ocrelizumab) is also approved for primary-progressive MS. In nearly all instances, these drugs are prescribed individually, so a patient only takes one DMT during any time period. Of these 15 approved drugs, eight are given at home via injection; four are given by a medical professional via intravenous (IV) infusion; and three are taken orally.
In brief, no clinical trial has shown convincing evidence of benefit in the treatment of primary progressive MS. All suggested treatments for PPMS are empiric. Several drugs that are more commonly used in the treatment of malignancy, cladribine and mitozantrone, appear to have some activity.
2 Secondary progressive MS, known as SPMS, begins as relapsed remitting disease and becomes progressive over time.
Available treatments of primary and secondary progressive MS are of limited efficacy and have significant side effects. An additional fact to consider is that most trials have not lasted longer than two or three years and give only hints about long-term results of treatment.
In brief, no clinical trial has shown convincing evidence of benefit in the treatment of primary progressive MS. All suggested treatments for PPMS are empiric. Several drugs that are more commonly used in the treatment of malignancy, cladribine and mitozantrone, appear to have some activity.
In contrast, there is definite modest benefit in some treatments for secondary progressive MS. These treatments include various regimens of steroid therapy (the anti-inflammatory effect) and the use of some drugs that modulate the immune system. Many of these drugs are more commonly used in treatment of cancer and rheumatoid arthritis such as cyclophosphamide, methotrexate and interferon.
MS should be treated by a neurologist who majors in MS with experience in managing it for years. The doctor with knowledge is so important regarding the specific disease. Do your research on experts treating this from NY to CA.
Remember the MS treatment is in parts to make up a whole plan:
1 Modifying the disease:
More than a dozen disease-modifying medications have been approved by the U.S. Food and Drug Administration (FDA) to treat relapsing forms of MS. These medications reduce the frequency and severity of relapses (also called attacks or exacerbations), reduce the accumulation of lesions in the brain and spinal cord as seen on magnetic resonance imaging (MRI) and may slow the accumulation of disability for many people with MS. No medications have yet been approved to treat primary-progressive MS.
2 Treating the Exacerbations:
An exacerbation of MS is caused by inflammation in the central nervous system (CNS) that causes damage to the myelin and slows or blocks the transmission of nerve impulses. To be a true exacerbation, the attack must last at least 24 hours and be separated from a previous exacerbation by at least 30 days. However, most exacerbations last from a few days to several weeks or even months. Exacerbations can be mild or severe enough to interfere with a person’s ability to function at home and at work. Severe exacerbations are most commonly treated with high-dose corticosteroids to reduce the inflammation.
3 Managing symptoms
In MS, damage to the myelin in the CNS and to the nerve fibers themselves interferes with the transmission of nerve signals between the brain and spinal cord and other parts of the body. This disruption of nerve signals produces the symptoms of MS, which vary depending on where the damage has occurred. MS symptoms can be effectively managed with a comprehensive treatment approach that includes medication(s) and rehabilitation strategies.
4 Promoting function through rehabilitation
Rehabilitation programs focus on function — they are designed to help you improve or maintain your ability to perform effectively and safely at home and at work. Rehabilitation professionals focus on overall fitness and energy management, while addressing problems with accessibility and mobility, speech and swallowing, and memory and other cognitive functions. Rehabilitation is an important component of comprehensive, quality healthcare for people with MS at all stages of the disease. Rehabilitation programs include cognitive and vocational rehabilitation, physical and occupational therapy, therapy for speech and swallowing problems, and more.
5 Providing emotional support
Comprehensive care includes attention to emotional health as well as physical health. Mental health professionals provide support and education, as well as diagnose and treat the depression, anxiety and other mood changes that are so common in MS. Neuropsychologists assess and treat cognitive problems.
MS is only part of overall health for a pt diagnosed with this disease! Comprehensive MS care is only a part — but not all — of a person’s overall health management strategies.
Like the general population, people with MS are subject to medical problems that have nothing to do with their MS — which means that regular visits with a primary care physician and age-appropriate screening tests are just as important for them as they are for everyone else. And the same goes for family members — your health and well-being are important too.

Updated 3/16/2023