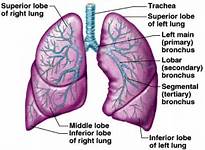
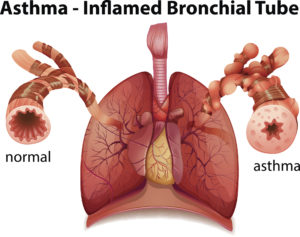
Asthma is a chronic, or long-term, disease that inflames and narrows the airways of your lungs
Asthma causes a variety of symptoms that can worsen at any time, making breathing difficult. Asthma is a disease that cannot be cured, but it can be managed. Some days you may not have symptoms, but this doesn’t mean your asthma has gone away. Asthma doesn’t have to slow you down. There are things you can do to control your asthma.
Asthma may cause the linings of your airways to get swollen, and the muscles around them can get tight. Sometimes the swelling and tightness get much worse. This is called an exacerbation, or asthma attack. An asthma attack can happen with any kind of asthma. Over time, effects of uncontrolled asthma, such as increased inflammation and asthma attacks, may have long-term effects on your breathing leading to permanent damage to the lining of your airways. Asthma attacks can be serious; that’s why it’s important for you to work with your healthcare provider to control your asthma.
Not all asthma is the same.
Asthma may be different for different people. Your healthcare provider may identify your type of asthma based on:
- how often you have symptoms
- nighttime awakenings
- how often you’re using your rescue inhaler
- if your asthma is keeping you from doing your normal activities
- how well you’re breathing, based on a breathing test
Your healthcare provider may assign the type of asthma that you have based on the most severe category listed above.
Intermittent asthma
If your asthma affects you twice a week or less, your asthma may be intermittent. You may need a rescue inhaler up to 2 days per week. It’s the mildest kind of asthma, but it’s not risk free, so be sure to tell your healthcare provider about your symptoms, and find out what you can do to help keep them under control.
Persistent asthma
Unlike intermittent asthma, with persistent asthma you may have symptoms and other limitations more often. Persistent asthma can be mild, moderate, or severe. Sometimes your symptoms may go away on their own. But other times, uncontrolled asthma may get worse. So can the risk of an asthma attack. It’s important to talk to your healthcare provider about your symptoms, and any changes you notice. Your healthcare provider can work with you to help control your asthma symptoms and reduce your risk.
People with mild asthma may have symptoms more than twice a week, but not every day. They may be awakened 3-4 times a month by their asthma or use a rescue inhaler called a SABA more than 2 days a week. They typically have some minor limits to their activities, but have a normal score on breathing tests. People with mild persistent asthma may also have some risk of asthma attacks that require corticosteroids (like prednisone).
If you have mild asthma, your doctor may prescribe a long-term controller medication like low-dose inhaled corticosteroids, as well as your rescue inhaler. When your mild asthma is well controlled, you may not have any symptoms at all, but this doesn’t mean your asthma has gone away.
If you have mild asthma, talk to your healthcare provider to make sure you are getting the right medicines to control your symptoms, and to help avoid asthma attacks. You should ask your healthcare provider what to watch for, and how to prevent an attack.
If you have severe asthma, you’re not alone. With the help of your doctor, severe asthma can be controlled. However, severe asthma affects roughly 5-10% of people with asthma. Uncontrolled severe asthma may include symptoms throughout the day, every day, or waking up every night due to asthma symptoms. You may need a rescue inhaler several times a day. People with severe asthma may have frequent asthma attacks that require oral corticosteroids, sometimes severe enough to send them to a hospital. Severe asthma may cause many limits to daily activities, and low scores on breathing tests.
Some risk factors that can play a part in whether you develop different types of asthma may include pollution, allergies, smoking, obesity, or genetics.
If your asthma is severe and uncontrolled, your healthcare provider may recommend a specialist, like an allergist or a pulmonary specialist (also called a pulmonologist). These doctors are specially trained to treat asthma. They can help you find the right combination of medication and self-care to help manage your