“PTSD can happen to anyone. It is not a sign of weakness. A number of factors can increase the chance that someone will have PTSD, many of which are not under that person’s control.”
U.S. Department of Veterans Affairs
“PTSD can happen to anyone. It is not a sign of weakness. A number of factors can increase the chance that someone will have PTSD, many of which are not under that person’s control.”
U.S. Department of Veterans Affairs
“Most people who have Crohn’s also have symptoms of ulcerative colitis but rectal bleeding, or blood in the stools, is much more common in people who have UC than those with Crohn’s. Because Crohn’s disease affects more of the body, it can cause some problems that doctors don’t usually see in people who have ulcerative colitis.”
WEB MD
“Calm the flame in your gut naturally.”
James Bogash DC (also Author of the book Chron’s Disease and Ulcerative Colitis)
“Treatments for coronary heart disease include heart-healthy lifestyle changes, medicines, medical procedures and surgery, and cardiac rehabilitation.”
National Heart, Lung and Blood Institute
Surgical procedure in which one or more blocked coronary arteries are bypassed by a blood vessel graft to restore normal blood flow to the heart. These graft usually come from the patient’s own arteries and veins located in the chest (thoracic), leg (saphenous) or arm (radial). The graft goes around the blocked artery (or arteries) to create new pathways for blood to flow to the heart.
Making a commitment to the following healthy lifestyle changes can go a long way toward promoting healthier arteries:
Various drugs can be used to treat coronary artery disease, including:
If you’ve had a heart attack, aspirin can help prevent future attacks. There are some cases where aspirin isn’t appropriate, such as if you have a bleeding disorder or you’re already taking another blood thinner, so ask your doctor before starting to take aspirin.
Sometimes more aggressive treatment is needed. Here are some options:
A stent is often left in the artery to help keep the artery open. Some stents slowly release medication to help keep the artery open.
Omega-3 fatty acids are a type of unsaturated fatty acid that’s thought to reduce inflammation throughout the body, a contributing factor to coronary artery disease. However, recent studies have not shown them to be beneficial. More research is needed.
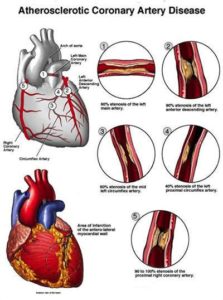

Coronary artery disease is thought to begin with damage or injury to the inner layer of a coronary artery, sometimes as early as childhood. The damage may be caused by various factors, including the following which are problems we can prevent or better control through better diet, some form of exercise balanced with rest. Including keeping our stress controlled in a productive way (like work out program to doing hobbies).
Causes that are modifiable (that we can change or help control):
Learn more tomorrow on treatment of CAD in Part III!
“The most common symptom of breast cancer is a new lump or mass, but other symptoms are also possible. It’s important to have any breast change checked by a health care provider.”
American Cancer Society
“Some human cells, including cancer cells, divide with a 24-hour rhythm. One of the main human circadian rhythm genes, cryptochrome, has been associated with diabetes and depression. Both of these discoveries grew from work with plants.”
Dr. Steven Kay (Biologist at the University of California)