Archive | August 2016
QUOTE FOR TUESDAY:
“Photosensitivity, sometimes referred to as a sun allergy, is an immune system reaction that is triggere.”
MERCK
QUOTE FOR MONDAY:
“More than one-third of adults and nearly 70% of children admit they’ve gotten sunburned within the past year, according to the CDC.”
WebM.D.
QUOTE FOR THURSDAY:
“Smoking cessation [stopping smoking] represents the single most important step that smokers can take to enhance the length and quality of their lives.”
The U.S. Surgeon General and American Cancer Society
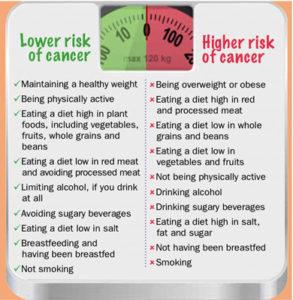
Control your weight as you quit smoking!
Not everyone gains weight when they stop smoking On average, people who quit smoking gain only about 10 pounds You are more likely to gain weight when you stop smoking especially if you stop smoking when you have smoked for 10 to 20 years or smoked one or more packs of cigarettes a day. You can control life. Although you might gain a few pounds, remember you have stopped smoking and taken a big step towards a healthier life.
What causes weight gain after quitting? When nicotine, a chemical n cigarette smoke, leaves your body, you may experience: Short-term weight gain. The nicotine kept your body weight low, and when you quit smoking your body returns to the weight it would have been had you never smoked.
You might gain 3-5 pounds due to water retention during the first week after quitting.
A need for fewer calories when quitting to smoke. After you stop smoking, you may use fewer calories than when you were smoking.
Will this weight gain hurt your health?
The health risks of smoking are far greater than the risks of gaining 5 to 10 pounds. Smoking causes more than 400,000 deaths each year in the United States. You would have to gain 100 to 150 lbs after quitting to make your health as high as when you smoked. The health risks of smoking and the benefits of quitting are listed below.
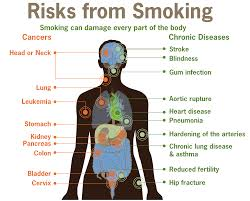
The Health Risks of Smoking
**Your Heart Rate Increases
**You expose yourself to some 4000 chemicals in cigarette smoke and 40 of these chemicals cause cancer.
**You are much more likely to get lung cancer compared to a nonsmoker. Men are 22 times more likely to develop lung cancer, while women who smoke are 12 times more likely.
**You are twice as likely to have a heart attack as a nonsmoker.
**You increase your risk for heart attack as a nonsmoker.
**You increase your risk for heart disease, stroke, some types of cancer (lung especially), emphysema, chronic bronchitis, and other lung diseases.
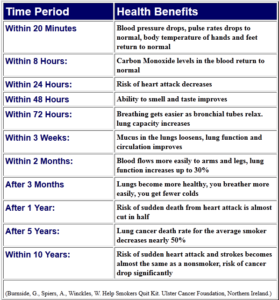
The Benefits of Quitting
When you quit smoking your body begins to heal from the effects of the nicotine within 12 hours after your last cigarette.
Your heart and lungs start repairing the damage caused by cigarette smoke.
You breathe easier and your smoker’s cough starts to go away.
You lower your risk for illness and death from heart disease, stroke, chronic bronchitis, emphysema, lung cancer, and other types of cancer.
You contribute to cleaner air, especially for children who are at risk for illnesses because they breathe others cigarette smoke.
Adapted from the National Cancer Institute’s “Smoking:Facts and Tips for Quitting”
QUOTE FOR WEDNESDAY:
“Because even healthy people can fall victim to summer heat, take the following precautions to reduce your risk:
-Drink plenty of water or other non-alcoholic beverages
-Wear lightweight, loose-fitting clothing that is light in color
-Reduce strenous activities or do them during the cooler parts of the day (not during 12pm-4pm the hottest time of a day).”
CDC Center for Disease Control and Prevention
QUOTE FOR TUESDAY:
” The most common types of breast cancer are ductal carcinoma in situ, invasive ductal carcinoma, invasive lobular carcinoma, medullary carcinoma, and Paget disease of the nipple (see definitions under these headings). “
American Cancer Society
Part II Breast Cancer
Can a healthy diet prevent breast cancer?
Eating a diet rich in fruits and vegetables hasn’t been consistently shown to offer protection from breast cancer. In addition, a low-fat diet appears to offer only a slight reduction in the risk of breast cancer.
However, eating a healthy diet may decrease your risk of other types of cancer, as well as diabetes, heart disease and stroke. A healthy diet can also help you maintain a healthy weight — a key factor in breast cancer prevention.
Is there a link between birth control pills and breast cancer?
A number of older studies suggested that birth control pills slightly increased the risk of breast cancer, especially among younger women. In these studies, however, 10 years after discontinuing birth control pills women’s risk of breast cancer returned to the same level as that of women who never used oral contraceptives. Current evidence does not support an increase in breast cancer with birth control pills.
Be vigilant about breast cancer detection. If you notice any changes in your breasts, such as a new lump or skin changes, consult your doctor. Also, ask your doctor when to begin mammograms and other screenings.
Once you’ve been diagnosed with breast cancer, your doctor works to find out the specifics of your tumor. Using a tissue sample from your breast biopsy or using your tumor if you’ve already undergone surgery, your medical team determines your breast cancer type. This information helps your doctor decide which treatment options are most appropriate for you.
Here’s what’s used to determine your breast cancer type.
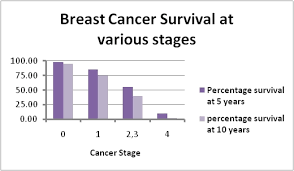
Is your cancer invasive or noninvasive?
Whether your cancer is invasive or noninvasive helps your doctor determine whether your cancer may have spread beyond your breast, which treatments are more appropriate for you, and your risk of developing cancer in the same breast or your other breast.
- Noninvasive (in situ) breast cancer. In situ breast cancer refers to cancer in which the cells have remained within their place of origin — they haven’t spread to breast tissue around the duct or lobule. One type of noninvasive cancer called ductal carcinoma in situ (DCIS) is considered a precancerous lesion. This means that if it were left in the body, DCIS could eventually develop into an invasive cancer. Another type of noninvasive cancer called lobular carcinoma in situ (LCIS) isn’t considered precancerous because it won’t eventually evolve into invasive cancer. LCIS does, however, increase the risk of cancer in both breasts.
- Invasive breast cancer. Invasive (infiltrating) breast cancers spread outside the membrane that lines a duct or lobule, invading the surrounding tissues. The cancer cells can then travel to other parts of your body, such as the lymph nodes. If your breast cancer is stage I, II, III or IV, you have invasive breast cancer.
In what part of the breast did your cancer begin?
The type of tissue where your breast cancer arises determines how the cancer behaves and what treatments are most effective. Parts of the breast where cancer begins include:
- Milk ducts. Ductal carcinoma is the most common type of breast cancer. This type of cancer forms in the lining of a milk duct within your breast. The ducts carry breast milk from the lobules, where it’s made, to the nipple.
- Milk-producing lobules. Lobular carcinoma starts in the lobules of the breast, where breast milk is produced. The lobules are connected to the ducts, which carry breast milk to the nipple.
- Connective tissues. Rarely breast cancer can begin in the connective tissue that’s made up of muscles, fat and blood vessels. Cancer that begins in the connective tissue is called sarcoma. Examples of sarcomas that can occur in the breast include phyllodes tumor and angiosarcoma.
- FYI a complication that can occur with advanced cancer that many of you may be unaware of. Bone metastasis occurs when cancer cells spread from their original site to a location in the bone. The most common types of cancer more likely to spread to bone include breast, prostate and lung cancers.Signs and symptoms of bone metastasis may include the following:
- Bone metastasis can occur in any bone, but more commonly occurs in the pelvis and spine. Bone metastasis may be the first sign that you have cancer, or it may occur years after your cancer treatment is completed, ex. Hodgkins Disease.
- Bone pain (back and pelvic pain are most common)
- Unexplained broken bones
- Loss of urine and/or bowel function
- Weakness in the legs
- High levels of calcium in the blood (hypercalcemia), which can cause nausea, vomiting and confusion
- The most common problem with metastatic bone cancer is pain and fractures. Metastatic bone cancer usually can’t be cured, but instead the goal is to provide pain relief and control further spread. Treatment can make a big difference and may include the following:
- Medications to repair and build new bone — These medications are similar to those used by people with osteoporosis and can help in building and strengthening your bone.
- Chemotherapy — Given as a pill or through a vein, used to control and treat cancer that has spread to the bone.
- Traditional radiation therapy — Radiation is given as external beam therapy to treat the cancer in the bone.
- Hormone therapy — Medications are used to block hormones (for breast and prostate cancers) that help control the spread of cancer to the bone.
- Surgery — Used to fix a fracture and stabilize a break from the cancer in the bone.
- Cryoablation — A special technique that freezes the cancer cells.
- Radiofrequency ablation — A special technique that heats the cancer cells.
- Chemoradiation — A form of internal radiation that is given through the vein and travels to the site of bone metastasis and targets the cancer cells.
- Pain medications — Medications provided with the goal of relieving and controlling pain from bone metastasis.
- Physical therapy — Exercises may be prescribed to assist in strengthening muscles and providing any assistive devices that may help you (cane, walker, crutches, etc.).If you’re living with metastatic bone cancer, you may find help and resources from a website called Bone Health in Focus. It was established with partners including BreastCancer.org, the National Lung Cancer Partnership and International Prostate Cancer Education & Support Network to offer resources that help patients and caregivers understand more about cancer that has spread to the bone (find the site at www.bonehealthinfocus.com).
- Are you living with cancer that has spread to the bone? Feel free to share your experiences with each other on the this blog striveforgoodhealth.com or on TheMayoclinic.org.
QUOTE FOR MONDAY:
“Be vigilant about breast cancer detection. If you notice any changes in your breasts, such as a new lump or skin changes, consult your doctor. Also, ask your doctor when to begin mammograms and other screenings.”
American Breast Cancer Society
QUOTE FOR THE WEEKEND:
“Some men with minimally enlarged prostate glands may experience symptoms while other men with much larger glands may have few symptoms. BPH is very common among older men, affecting about 60% of men over age 60 and 80% of men over age 80. Recommended to start yearly annual BPH visits to the doctor at age 50.”
University of Maryland-School of Medicine.