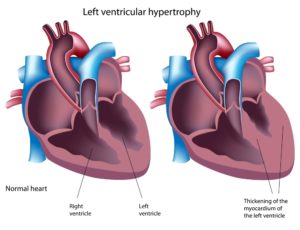
 Left Ventricle Enlarged
Left Ventricle Enlarged
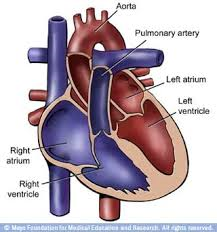 Normal Heart Size & Lt.Ventricle
Normal Heart Size & Lt.Ventricle
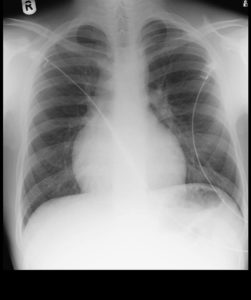 Heart Enlarged
Heart Enlarged

Think of a healthy heart like a firm biceps muscle. An enlarged heart is just the opposite.
When your heart is enlarged, it’s like a soft biceps — it’s weak and out of shape. What happens is the heart muscle enlarges because the heart is trying so hard to do its function, PUMP, but it gets too difficult and the muscle of the heart enlarges/thickens causing the organ not to work properly. So this causes back up with circulatory blood, think like a plumber–your pipes are backing up. So what does this ends up causing? Your body starts to retain fluid, your lungs get congested with fluid and your heart begins to beat irregularly. If the heart is effected in working so will the lungs in time and visa versa. Think like the car if the engine (the heart) is effected working properly the transmission (the lungs) will be also in time.
“In general the term ‘enlarged heart’ refers to heart failure,” said Clyde Yancy, M.D., past president of the American Heart Association and chief of the Division of Cardiology and the Magerstadt Professor of Medicine at Northwestern University Feinberg School of Medicine in Chicago. “This is a common condition that’s more likely to occur in older patients. It’s most strongly related to a history of high blood pressure or a previous heart attack.”
About one in five adults over age 40 is affected, with African-Americans facing a greater risk due to the dieting and heridity. Take high blood pressure as a major risk factor since
Cardiosmart American College of Cardiology say in 2018 “Black adults are up to two times more likely to develop high blood pressure by age 55 compared to whites, with many of these racial differences developing before age 30, concludes a study recently published in the Journal of the American Heart Association.”.
“There are other reasons for an enlarged heart or heart muscle disorders (like cardiomyopathies, which are diseases of the heart muscle) and not everyone with heart failure has an enlarged heart,” Dr. Yancy said. “But when we speak of an enlarged heart we are typically referring to heart failure.”
What to Look For
Shortness of breath, fluid retention (edema) and having a harder time exercising are among the key symptoms of an enlarged heart or heart failure. Irregular heartbeats (arrhythmias) — potentially even serious irregular heart rhythms and strokes — are likely as well, Dr. Yancy said.
The symptoms of an enlarged heart can affect the quality and length of your life, Dr. Yancy said.
“This is why treatment is so important and why we are so encouraged that good treatments are available today,” he said.
How to Prevent and Treat It
“Despite all of the great advances in treatment, the best treatment is to never have an enlarged heart,” Dr. Yancy said. “Prevention should be the true thrust. The simple stuff works — managing your weight, getting plenty of physical activity, controlling your diet, reducing your cholesterol and avoiding diabetes.”
But there’s good news for those who have been diagnosed with an enlarged heart.
“Whereas this condition was a dreadful diagnosis 20–25 years ago and resulted in death shortly afterward, the outlook for those with heart failure is now so much better,” Dr. Yancy said. “More and more patients are living longer, healthier lives with heart failure due to breakthrough medical and device treatments.”
If you or a loved one has heart failure, seek a care provider who has experience treating enlarged hearts.
“This condition is no longer about ‘failure,’” Dr. Yancy said. “On the correct drugs and with support from the correct devices, you can be successful in overcoming heart failure.” Dr. Yancy said there’s a nationwide “small army” of expert nurses focusing on heart failure.
”When a heart failure nurse is involved, you can expect to get better — a lot better,” he said.
Drugs and devices can strengthen the heart, and pacemakers and implantable defibrillators (ICDs) also offer hope. Surgery may be another option for patients who also have heart vessel disease and /or heart valve disease. “For those with very advanced disease, we now have very effective mechanical heart devices and we do heart transplantation very well,” he said.
And the future may hold more promise for enlarged hearts, Dr. Yancy said.
“We expect to have cell-based therapies that will help us repair damaged hearts; easier surgeries that will halt the progression of heart disease and even more insight into preventing heart disease,” he said.
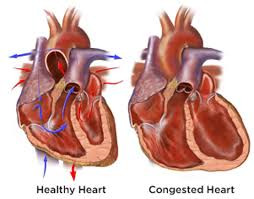
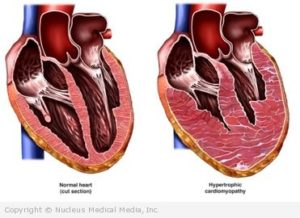


 Left Ventricle Enlarged
Left Ventricle Enlarged Normal Heart Size & Lt.Ventricle
Normal Heart Size & Lt.Ventricle Heart Enlarged
Heart Enlarged