Overview
Traumatic brain injury (TBI) is sudden damage to the brain caused by a blow or jolt to the head. Common causes include car or motorcycle crashes, falls, sports injuries, and assaults. Injuries can range from mild concussions to severe permanent brain damage. While treatment for mild TBI may include rest and medication, severe TBI may require intensive care and life-saving surgery. Those who survive a brain injury can face lasting effects in their physical and mental abilities as well as emotions and personality. Most people who suffer moderate to severe TBI will need rehabilitation to recover and relearn skills.
What is a traumatic brain injury?
TBI is an injury to the brain caused by a blow or jolt to the head from blunt or penetrating trauma. The injury that occurs at the moment of impact is known as the primary injury. Primary injuries can involve a specific lobe of the brain or can involve the entire brain. Sometimes the skull may be fractured, but not always. During the impact of an accident, the brain crashes back and forth inside the skull causing bruising, bleeding, and tearing of nerve fibers (Fig. 1). Immediately after the accident the person may be confused, not remember what happened, have blurry vision and dizziness, or lose consciousness. At first the person may appear fine, but their condition can decline rapidly. After the initial impact occurs, the brain undergoes a delayed trauma – it swells – pushing itself against the skull and reducing the flow of oxygen-rich blood. This is called secondary injury, which is often more damaging than the primary injury.

Figure 1. During impact to the head, the soft brain crashes back and forth against the inside of the hard skull causing bruising, bleeding, and shearing of the brain.
Traumatic brain injuries are classified according to the severity and mechanism of injury:
- Mild: person is awake; eyes open. Symptoms can include confusion, disorientation, memory loss, headache, and brief loss of consciousness.
- Moderate: person is lethargic; eyes open to stimulation. Loss of consciousness lasting 20 minutes to 6 hours. Some brain swelling or bleeding causing sleepiness, but still arousable.
- Severe: person is unconscious; eyes do not open, even with stimulation. Loss of consciousness lasting more than 6 hours.
Types of traumatic brain injuries
- Concussion is a mild head injury that can cause a brief loss of consciousness and usually does not cause permanent brain injury.
- Contusion is a bruise to a specific area of the brain caused by an impact to the head; also called coup or contrecoup injuries. In coup injuries, the brain is injured directly under the area of impact, while in contrecoup injuries it is injured on the side opposite the impact.
- Diffuse axonal injury (DAI) is a shearing and stretching of the nerve cells at the cellular level. It occurs when the brain quickly moves back and forth inside the skull, tearing and damaging the nerve axons. Axons connect one nerve cell to another throughout the brain, like telephone wires. Widespread axonal injury disrupts the brain’s normal transmission of information and can result in substantial changes in a person’s wakefulness.
- Traumatic Subarachnoid Hemorrhage (tSAH) is bleeding into the space that surrounds the brain. This space is normally filled with cerebrospinal fluid (CSF), which acts as a floating cushion to protect the brain. Traumatic SAH occurs when small arteries tear during the initial injury. The blood spreads over the surface of the brain causing widespread effects.
- Hematoma is a blood clot that forms when a blood vessel ruptures. Blood that escapes the normal bloodstream starts to thicken and clot. Clotting is the body’s natural way to stop the bleeding. A hematoma may be small or it may grow large and compress the brain. Symptoms vary depending on the location of the clot. A clot that forms between the skull and the dura lining of the brain is called an epidural hematoma. A clot that forms between the brain and the dura is called a subdural hematoma. A clot that forms deep within the brain tissue itself is called an intracerebral hematoma. Over time the body reabsorbs the clot. Sometimes surgery is performed to remove large clots.
Although described as individual injuries, a person who has suffered a TBI is more likely to have a combination of injuries, each of which may have a different level of severity. This makes answering questions like “what part of the brain is hurt?” difficult, as more than one area is usually involved.
Secondary brain injury occurs as a result of the body’s inflammatory response to the primary injury. Extra fluid and nutrients accumulate in an attempt to heal the injury. In other areas of the body, this is a good and expected result that helps the body heal. However, brain inflammation can be dangerous because the rigid skull limits the space available for the extra fluid and nutrients. Brain swelling increases pressure within the head, which causes injury to parts of the brain that were not initially injured. The swelling happens gradually and can occur up to 5 days after the injury.
What are the symptoms?
Depending on the type and location of the injury, the person’s symptoms may include:
- Loss of consciousness
- Confusion and disorientation
- Memory loss / amnesia
- Fatigue
- Headaches
- Visual problems
- Poor attention / concentration
- Sleep disturbances
- Dizziness / loss of balance
- Irritability / emotional disturbances
- Feelings of depression
- Seizures
- Vomiting
Diffuse injuries (such as a concussion or diffuse axonal injury) will typically cause an overall decreased level of consciousness. Whereas, focal injuries (such as an ICH or a contusion) will have symptoms based on the brain area affected (Fig. 2).
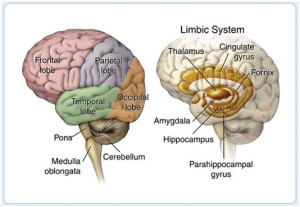
Lobes of the brain that can get affected by TBI:
Figure 2. The brain is composed of three parts: the brainstem, cerebellum, and cerebrum, which is divided into lobes. The table lists the lobes of the brain and their normal functions as well as problems that may occur when injured. While an injury may occur in a specific area, it is important to understand that the brain functions as a whole by interrelating its component parts.
Every patient is unique and some injuries can involve more than one area or a partial section, making it difficult to predict which specific symptoms the patient will experience.






 4 days ago
4 days ago