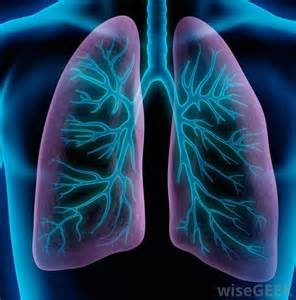
When you breathe in, air enters through your mouth and nose and goes into your lungs through the trachea (windpipe). The trachea divides into tubes called the bronchi (singular, bronchus), which enter the lungs and divide into smaller branches called the bronchioles. At the end of the bronchioles are tiny air sacs known as alveoli.
Many tiny blood vessels run through the alveoli. They absorb oxygen from the inhaled air into your bloodstream and pass carbon dioxide (a waste product from the body) into the alveoli. This is expelled from the body when you exhale. Taking in oxygen and getting rid of carbon dioxide are your lungs’ main functions.
A thin lining called the pleura surrounds the lungs. The pleura protects your lungs and helps them slide back and forth as they expand and contract during breathing. The space inside the chest that contains the lungs is called the pleural space (or pleural cavity).
Below the lungs, a thin, dome-shaped muscle called the diaphragm separates the chest from the abdomen. When you breathe, the diaphragm moves up and down, forcing air in and out of the lungs.
LUNG CANCER
There are 3 types of lungs cancer. The two most common types of lung cancer that exist are 1 non-small cell lung cancer (NSCLC), which is the most common, and 2 small cell lung cancer (SCLC), an aggressive cancer that occurs in just over 10 percent of all lung cancer cases.
The third group is 3 lung carcinoid tumors (also known as lung carcinoids) are a type of lung cancer, which is a cancer that starts in the lungs. Cancer starts when cells begin to grow out of control. Cells in nearly any part of the body can become cancer, and can spread to other areas of the body.
Lung carcinoid tumors are uncommon and tend to grow slower than other types of lung cancers. They are made up of special kinds of cells called neuroendocrine cells.
Lung Cancer Symptoms
Both major types of lung cancer have similar symptoms. These symptoms often include a cough that doesn’t go away and shortness of breath.
Sometimes lung cancer does not cause any signs or symptoms. It may be found during a chest X-ray done for another condition. Signs and symptoms may be caused by lung cancer or by other conditions. Check with your doctor if you have any of the following:
- Chest discomfort or pain
- A cough that doesn’t go away or gets worse over time
- Trouble breathing
- Wheezing
- Blood in sputum (mucus coughed up from the lungs)
- Hoarseness
- Loss of appetite
- Weight loss for no known reason
- Tiredness/lethargy
- Trouble swallowing
- Swelling in the face and/or veins in the neck
For both conditions, early detection through a low-dose computed topography (CT) scan is especially critical. Identifying lung cancer in its earliest stages even before you have symptoms can reduce the risk of death by 20 percent, according to recent studies.
Non-small cell lung Cancer (NSCLC)
Non-small cell lung cancer (NSCLC) is the most common type of cancer in lung tissues. Your risk of developing this disease increases if you are a longtime or former smoker, have been exposed to passive smoke, or have had environmental or occupational exposure to radon, asbestos, uranium, and other substances. The primary types of NSCLC are named for the type of cells found in the cancer:
- Squamous-cell carcinoma (also called epidermoid carcinoma)
- Adenocarcinoma
- Large-cell carcinoma
- Adenosquamous carcinoma
- Undifferentiatiated carcinoma
Small Cell Lung Cancer (SCLC)
In small cell lung cancer (SCLC), small cancerous cells arise in the airway, usually in a central location. This is an aggressive cancer that spreads quickly throughout the body through the blood and lymphatic (node) systems. Typically occurring in people who smoke or who used to smoke, SCLC accounts for just over 10 percent of all lung cancers.


